Katherine Buck, MD, awarded a prestigious grant to design a diagnostic pathway for pneumonia in older adults
In older adults, pneumonia can be an elusive illness. Although more than 500,000 patients are treated for pneumonia each year in emergency departments (ED), physicians still struggle to accurately diagnose the infection.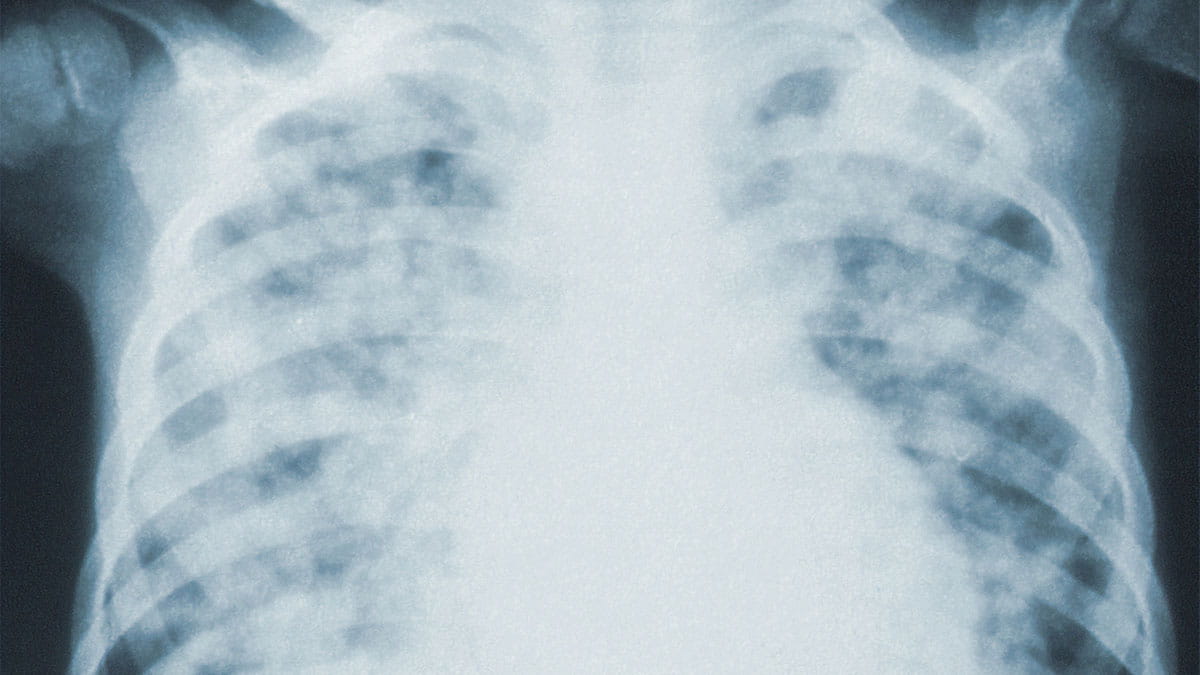
Many factors contribute to this challenge, including unusual symptoms, comorbidities, inaccurate chest x-rays and unreliable biomarkers to detect the disease. When physicians fail to diagnose older adults with pneumonia, patients may face inadequate treatment, leading to a worsening infection that could eventually become fatal.
To improve pneumonia mortality rates in older adults, Katherine Buck, MD, assistant professor of Emergency Medicine at The Ohio State University College of Medicine, was awarded a $1.2 million National Institute on Aging K76 Paul Beeson Career Development Award for her new project, “Establishing and Implementing Pneumonia Diagnosis in ED Older Adults: A Mixed Methods Approach.” This project, which is a funding collaboration between the National Institute on Aging, the American Federation for Aging Research and the John A. Hartford Foundation, aims to lay the groundwork for ED physicians to diagnose pneumonia more accurately.
“Unfortunately, pneumonia is a hard diagnosis in older adults in the ED for many reasons. Both over and under-diagnosis have potential consequences,” Dr. Buck says. “Thus, we need to improve diagnostic accuracy with the results available, which are sometimes limited, and within the limitations of these results. The goal is to produce a diagnostic pathway for physicians to follow that improves diagnostic accuracy.”
To create a diagnostic pathway, or a set of steps and criteria that help a physician make a diagnosis, one central goal of Dr. Buck’s project includes analyzing two new tests that could diagnose pneumonia. One of these tests involves antimicrobial peptides (AMPs), which are small molecules that respond to bacteria and viruses as part of the innate immune system. AMPs could allow physicians to detect bacterial and viral pathogens, both of which can cause pneumonia. The second test, called monocyte distribution width (MDW), measures the size of white blood cells in the patient’s body, as well as any increases in ED sepsis that could indicate infection. Dr. Buck’s project will investigate how effective these tests are in combination with patients’ symptoms and existing diagnostic tools for diagnosing pneumonia in older individuals.
After developing the groundwork for the pneumonia diagnostic pathway, Dr. Buck and her team plan to consult ED physicians about how this pathway could be successfully implemented, specifically focusing on potential facilitators and barriers in emergency medicine. To do this, the project utilizes a technique called Group Concept Mapping.
“Group Concept Mapping is a mixed-methods (both qualitative and quantitative) analytic technique driven by the participants who are the stakeholders. In this case, emergency physicians,” Dr. Buck says. “In this project, it will collect data about what attributes of clinical decision rules are important to emergency physicians. The goal is to use this information to guide the development of our clinical diagnostic pathway so that it is a tool emergency physicians want to use.”
Dr. Buck hopes that the pneumonia diagnostic pathway shaped by novel testing methods and group concept mapping will yield a strong foundation for applying this pathway in emergency medicine, leading to enhanced treatment and decreasing mortality for ED patients.
“The most exciting thing to me is that this is a real and common problem we face in the emergency department and, if we are successful, the results could immediately improve patient care,” Dr. Buck says.