The story behind the Ohio State College of Medicine’s rise in U.S. News & World Report rankings
It’s been a remarkable year at The Ohio State University College of Medicine, and the 2022 U.S. News & World Report medical school rankings reflect that. Ohio State moved up a spot to become the 33rd best medical school in research, and climbed 10 spots to be the 28th medical school in primary care.
In a new category, the Ohio State College of Medicine debuted as the 7th most diverse medical school, the highest ranking among the top 40 research schools. Additionally, three of our specialties programs were ranked: Surgery as 17, Anesthesiology as 18 and Pediatrics as 21.
The climb in 2022 rankings demonstrates the Ohio State College of Medicine’s dedication to relentless improvement and discovery—but numbers only tell a part of the story.
2020 was a year when the Ohio State College of Medicine tackled the COVID-19 pandemic while continuing to push the boundaries of health education and research across medical disciplines. It was a year in which the college welcomed a new dean, expanded its powerhouse neuroscience programs and made telehealth an invaluable tool in primary care and beyond. Learning continued in earnest, in some cases with even greater urgency—from core fundamentals to the latest technological advancements, students and residents developed the vital skills needed to take on the world’s most common and pressing health challenges.
Whether through the discovery of timely solutions or the continued elevation of the college’s strengths in research and education, here are a few reasons the Ohio State College of Medicine stood out among its peers in 2020—and where it’s headed in 2021 and beyond.
Recruiting world-class leaders and pushing the boundaries of research and care
 Dean Bradford joins the College of Medicine: In August, The Ohio State University welcomed a strong academic leader and well-known physician-scientist in the field of Otolaryngology – Head and Neck Surgery to lead the College of Medicine.
Dean Bradford joins the College of Medicine: In August, The Ohio State University welcomed a strong academic leader and well-known physician-scientist in the field of Otolaryngology – Head and Neck Surgery to lead the College of Medicine.
“I came to The Ohio State University College of Medicine because it is on a trajectory like no other in academic medicine,” says Carol R. Bradford, MD, MS, FACS. “There is tremendous transformation, discovery and innovation happening in Columbus, and I am excited to be part of it.”
Dr. Bradford became the 15th dean of the medical college and vice president for Health Sciences, joining Ohio State from the University of Michigan, where she was executive vice dean of academic affairs and the chief academic officer for Michigan Medicine. In September, she became the president of the American Academy of Otolaryngology – Head and Neck Surgery.
Answering our biggest COVID-19 questions: In September, researchers at the Ohio State College of Medicine and the Ohio State Wexner Medical Center were awarded a five-year, $10 million grant from the National Cancer Institute to study the impact of COVID-19 on first responders, health care workers and the general population.
The grant, one of the largest ever awarded to the Ohio State College of Medicine, is funding the Center for Serological Testing to Improve Outcomes from Pandemic COVID-19 (STOP-COVID) at Ohio State, a new Serological Sciences Center of Excellence. The center uses state-of-the-art serological and molecular tests developed at the Ohio State Wexner Medical Center, and researchers across disciplines are exploring the interactions among exposure risks, transmission, immune responses, disease severity, protection and barriers to COVID-19 testing and vaccination.
“Stopping the spread of COVID-19 will require research that cross-cuts basic, translational and applied sciences,” said Eugene Oltz, PhD, chair of the Department of Microbial Infection and Immunity and lead co-principal investigator for this study.
Nearly 2,000 participants are projected to be followed over the five-year period.
A swiftly growing neuroscience effort: Throughout 2020, Ohio State’s powerhouse neuroscience programs continued building their world-class institute dedicated to the treatment of patients with neurological and psychiatric disorders.
Ohio State’s Neurological Institute, which houses over 200 medical, surgical and research specialists, is one of the country’s first efforts to combine several neuroscience-related specialties into one program to tackle the world’s most pressing health challenges of the brain, spine, nerves and muscle.
“Anybody can form a neurological institute, but the advantages unique to Ohio State are the individuals involved, from scientists to staff,” says Russell Lonser, MD, chair of the Department of Neurological Surgery and co-chair of the Neurological Institute. “We’re a massive university with incredible resources and talented individuals coming together in a very intentional way.”
 A swift expansion of telehealth: With COVID-19 keeping many home, Ohio State launched a blitz of telehealth training and deployed technology to enable remote visits. In just 10 days at the start of the pandemic, the percentage of Ohio State clinicians across all specialties conducting telehealth visits skyrocketed from 2% to more than 95%.
A swift expansion of telehealth: With COVID-19 keeping many home, Ohio State launched a blitz of telehealth training and deployed technology to enable remote visits. In just 10 days at the start of the pandemic, the percentage of Ohio State clinicians across all specialties conducting telehealth visits skyrocketed from 2% to more than 95%.
“A major part of our mission is to improve people's lives, and we realized if we couldn’t reach out to patients in their homes, we couldn’t help them,” says L. Arick Forrest, MD, MBA, vice dean of Clinical Affairs for the Ohio State College of Medicine. “This was the way we could connect to so many of our patients, whether they needed care for a common sinus infection or a consultation for a complex gastrointestinal problem.”
These remote visits covered a wide range of primary care needs and also helped specialists maintain patient relationships and conduct electronic consultations with primary care clinicians for seamless specialty care. The learnings from the COVID-19 era of telehealth will inform the future of the broader telehealth program at Ohio State, both in its practice and teaching of future physicians.
Finding thoughtful, timely answers to today’s urgent challenges
 Diversity, equity and inclusion in education: Outside of historically black colleges and universities, the Ohio State College of Medicine is one of the top medical schools in the nation for its percentage of Black students. But while the college may be ahead of the curve in admitting underrepresented students, its faculty and leaders recognize the challenge in giving those minorities the support and resources they need to feel welcome and to be successful in their careers.
Diversity, equity and inclusion in education: Outside of historically black colleges and universities, the Ohio State College of Medicine is one of the top medical schools in the nation for its percentage of Black students. But while the college may be ahead of the curve in admitting underrepresented students, its faculty and leaders recognize the challenge in giving those minorities the support and resources they need to feel welcome and to be successful in their careers.
“There needs to be a collaborative and cooperative effort by many at every single layer of an organization to actively and deliberately address the issues of systemic racism that have been woven, intentionally or unintentionally, into policies, practices and culture,” says Demicha Rankin, MD, associate dean of Admissions.
In 2020, the college formed an Equity and Anti-Racism Task Force, a multidisciplinary group of 10 faculty and seven students aimed at better addressing the unique needs of MD students from backgrounds underrepresented in medicine, and supporting cultural competency for all. The college is reassessing how faculty teach racism as a public health crisis and testing the success of mentorship pairings with faculty and students from similar backgrounds.
Rapid solutions for COVID-19: The COVID-19 pandemic presented some massive challenges—as well as opportunities to put research discoveries into action immediately.
“This is what distinguishes academic medical centers,” says Peter Mohler, PhD, vice dean of Research at the Ohio State College of Medicine. “Their work is in the spotlight in 2020. And COVID-19 solutions are being rapidly developed at Ohio State.”
Collaboration among Ohio State’s seven health science colleges, across the university and The Ohio State University Wexner Medical Center in 2020 led to swift solutions that saved lives nationwide. Researchers and clinicians worked to improve and expand COVID-19 testing; increase the supply of personal protective equipment; and develop, overnight, an in-house “recipe” for the sterile solution needed to hold test swabs.
As a growing abundance of vaccines deliver new promise in the fight against COVID-19, the Ohio State College of Medicine’s COVID-19-related work continues through more than 100 research projects.
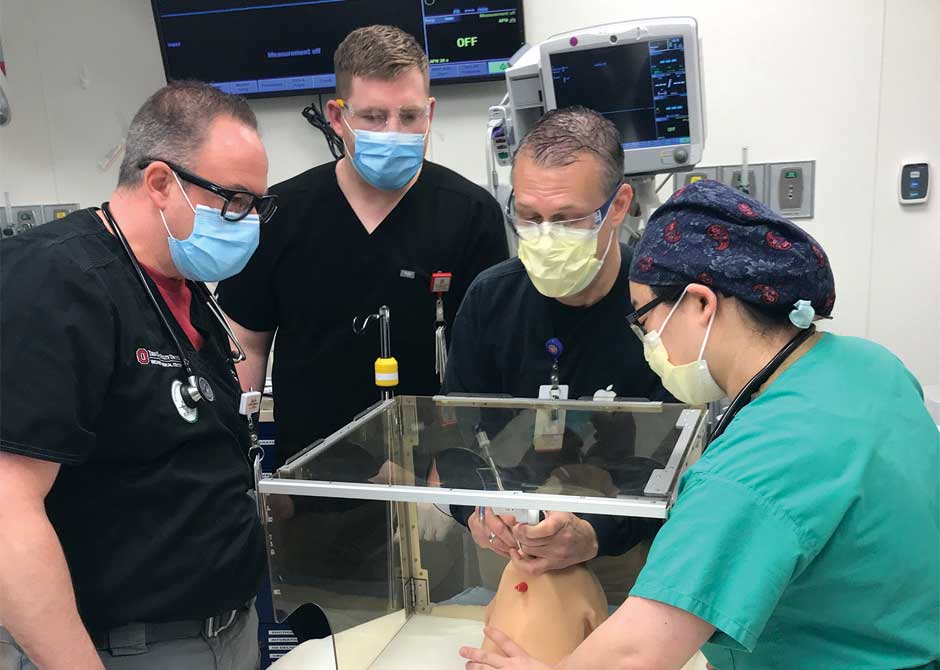 Disaster medicine in the pandemic age: “Today, disaster response requires a different mindset,” says Nicholas Kman, MD, professor of Emergency Medicine at the Ohio State College of Medicine. “We must move from a mode of taking care of individual patients to taking care of the population as a whole. So we had to redesign our course.”
Disaster medicine in the pandemic age: “Today, disaster response requires a different mindset,” says Nicholas Kman, MD, professor of Emergency Medicine at the Ohio State College of Medicine. “We must move from a mode of taking care of individual patients to taking care of the population as a whole. So we had to redesign our course.”
A massive interdisciplinary collaboration in 2020 led to the expedited creation of “Pandemic and Disaster Medicine: COVID-19 Response From the Bedside to the Federal Level,” which was initially offered to graduating seniors and other medical students who—like fellow trainees across the nation—had been locked out of traditional third-and fourth-year clinical rotations due COVID-19 precautionary safety measures.
Designed to develop critical thinking and judgment skills, the course uses an incident response playbook that models the spread of an infectious disease as well as scenarios that Dr. Kman implemented during COVID-19. It teaches medical students not only best practices for disaster management but also how to manage the psychosocial pressures of caring for large numbers of patients with serious medical issues.
“At Ohio State, we’ve been teaching disaster medicine for some time now,” says Daniel Clinchot, MD, vice dean for Education. “But our team’s ability to quickly pivot to COVID-19 education allows our students to gain strong pandemic skills, so they’re fully prepared to enter the real world and offer expertise as new graduates.”
Driving innovations in fundamental and advanced education
New environments propel interdisciplinary learning: Progress continues on the Interdisciplinary Health Sciences Center, the new home of the Ohio State College of Medicine that will transform learning and foster a new, integrated model for health care education where students from all health science disciplines learn together.
Construction began in 2019 on this complex, which includes a 150,000-square-foot renovation of Hamilton Hall and construction of a 100,000-square-foot building to create an interdisciplinary, technology-rich campus for collaborative learning. The center is scheduled to open in three phases, beginning in 2022.
The reimagined Ohio State College of Medicine is part of a $3 billion campuswide transformation at the university that includes a cascade of new construction: an 820-bed inpatient hospital, a 270,000-square-foot Interdisciplinary Research Center, a sterile supply building, and outpatient care centers strategically located throughout central Ohio.
 Sophisticated simulations for essential skills: The Ohio State College of Medicine is one of a small handful of schools to integrate KindHeart into its cardiothoracic surgery program, employing a simulator that uses a pig’s heart attached to balloons to keep it beating and stage blood to simulate bleeding.
Sophisticated simulations for essential skills: The Ohio State College of Medicine is one of a small handful of schools to integrate KindHeart into its cardiothoracic surgery program, employing a simulator that uses a pig’s heart attached to balloons to keep it beating and stage blood to simulate bleeding.
The simulation doesn’t replace experiences with human patients, but it creates an environment of deliberate practice and repetition to develop muscle-memory skills necessary for excellent surgeons—even under heavy stress.
“It’s an important complementary process—what we can do in the simulation lab, we can’t do on real patients,” says Nahush Mokadam, MD, a professor and director of the Ohio State Division of Cardiac Surgery and the program director for Ohio State’s Cardiothoracic Surgery Fellowship. “We can operate until residents get it right.”
A game-changing ultrasound program: Ultrasound isn’t new, but few clinicians are trained to acquire and interpret ultrasound images. That’s where the Ohio State College of Medicine is different—it trains medical students early in their first year to harness the power of ultrasound, giving them measurable advantages, particularly in emergent situations. About 800 students learn ultrasound techniques every year through an integrated, mandatory curriculum.
“It helps our students better master the first-year content, integrating anatomy and physiology, and learning it dynamically in real time,” says Creagh Boulger, MD, associate director of Ultrasound and an associate professor of Emergency Medicine. “They get early exposure to clinical skills and spend one-to-one time with practicing physicians so that they begin to apply clinical skills and think like doctors earlier.”
This builds “phenomenal residents” who find themselves head-and-shoulders above their peers, Dr. Boulger says. “I’ve watched our students enter residency with a solid foundation and clinical acumen because they’ve been exposed early to ultrasound in clinical scenarios. They hit the ground running.”
Enhance understanding of inequities: Trainees and practicing clinicians alike are learning how to provide better care for their most vulnerable patients through virtual reality-based simulations created in partnership with the Ohio Department of Medicaid and the Ohio Colleges of Medicine Government Resource Center.
The goal of the training programs isn’t just to increase knowledge, but to increase understanding and empathy among care providers, says Sheryl Pfeil, MD, medical director of the Ohio State College of Medicine’s Clinical Skills Center.
“It imparts not so much how to be a dentist or how to treat back pain, but it’s teaching us how to provide better, more culturally sensitive care for patients in all sorts of circumstances,” Dr. Pfeil says. “Frankly, it’s what we must strive to do as physicians.”
The future of an academic medicine powerhouse
 Every day, the Ohio State College of Medicine’s more than 4,500 learners, nearly 2,400 faculty members and thousands of staff members fulfill each facet of their mission to improve lives—starting with the nearly 2 million people in central Ohio and reaching beyond to the entire state, the Midwest, the nation and the world.
Every day, the Ohio State College of Medicine’s more than 4,500 learners, nearly 2,400 faculty members and thousands of staff members fulfill each facet of their mission to improve lives—starting with the nearly 2 million people in central Ohio and reaching beyond to the entire state, the Midwest, the nation and the world.
For the Ohio State College of Medicine, these are only a few of the highlights from 2020—and a mere hint at where the college is headed in the years to come.



