ASH Award sheds light on student research in multiple myeloma
 Second-year Ohio State University medical student Jordan Nunnelee is the proud recipient of an Abstract Achievement Award presented by the American Society of Hematology (ASH) in recognition of his research titled Improvement in Survival of Multiple Myeloma Patients: A Long-Term Institutional Experience. The ASH award will pay for Jordan’s trip to Orlando, Florida in early December to attend the society’s annual meeting and present his award-winning abstract.
Second-year Ohio State University medical student Jordan Nunnelee is the proud recipient of an Abstract Achievement Award presented by the American Society of Hematology (ASH) in recognition of his research titled Improvement in Survival of Multiple Myeloma Patients: A Long-Term Institutional Experience. The ASH award will pay for Jordan’s trip to Orlando, Florida in early December to attend the society’s annual meeting and present his award-winning abstract.
As described in his abstract, the study sought to determine trends in survival of patients with multiple myeloma (MM) since 1992 at The OSU Comprehensive Cancer Center. MM is a cancer of the blood in which plasma cells in the bone marrow become cancerous and grow out of control, crowding out normal blood-forming cells and leading to low blood counts, increased bruising and bleeding, difficulty fighting infection, and other conditions. MM represents 1.8% of all new cancer cases in the U.S., with an estimated 32,110 new cases in 2019, according to the National Cancer Institute.
Looking at patients since 1992, the research examined long-term survival as new therapies emerged to treat patients with MM, administered before and after autologous transplantation (ASCT). ASCT is a treatment in which the patient’s own blood-forming stem cells are collected, stored, and returned after the cancer cells are destroyed.
“With the introduction of new and more effective drugs used before and after ASCT, we performed survival analysis in [Newly Diagnosed Multiple Myeloma] NDMM patients from 1992 to 2016 receiving ASCT to examine our institutional progress,” explains Jordan.
Analyzing data gathered from Medical Center records of 1002 patients with a case history of MM, the team was able to identify and categorize the data based on historical changes in novel agents, and determine how survival has improved over time, likely due to these novel agents.
The study revealed a correlation between more recent transplants where more “advanced” therapies were used and improvement in survival rates. There were also notable improvements in survival among other specific patient groups, such as elderly patients (over age 65) and genetically high-risk patients.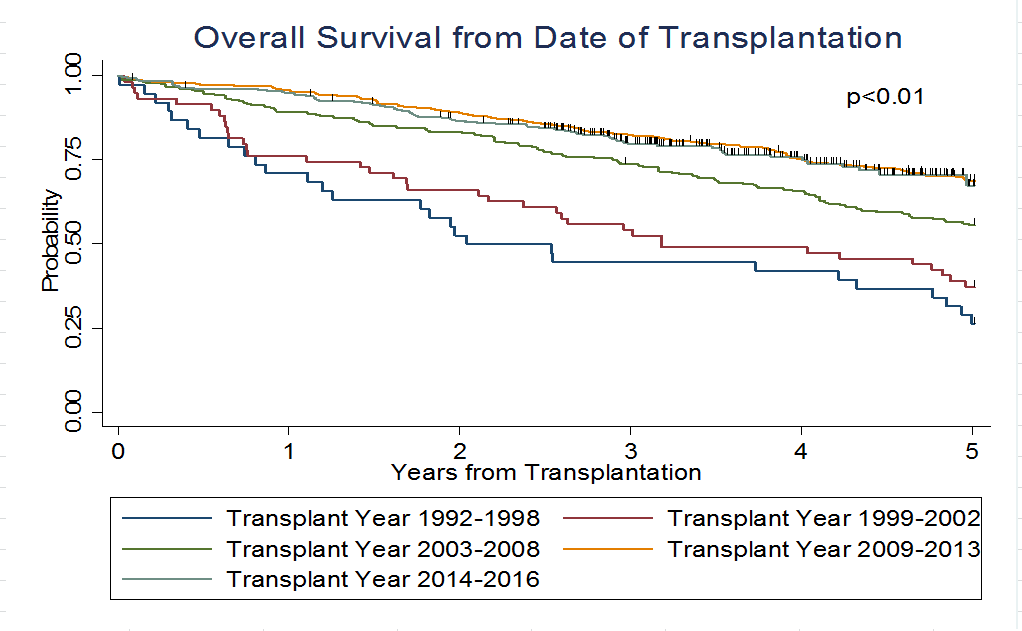
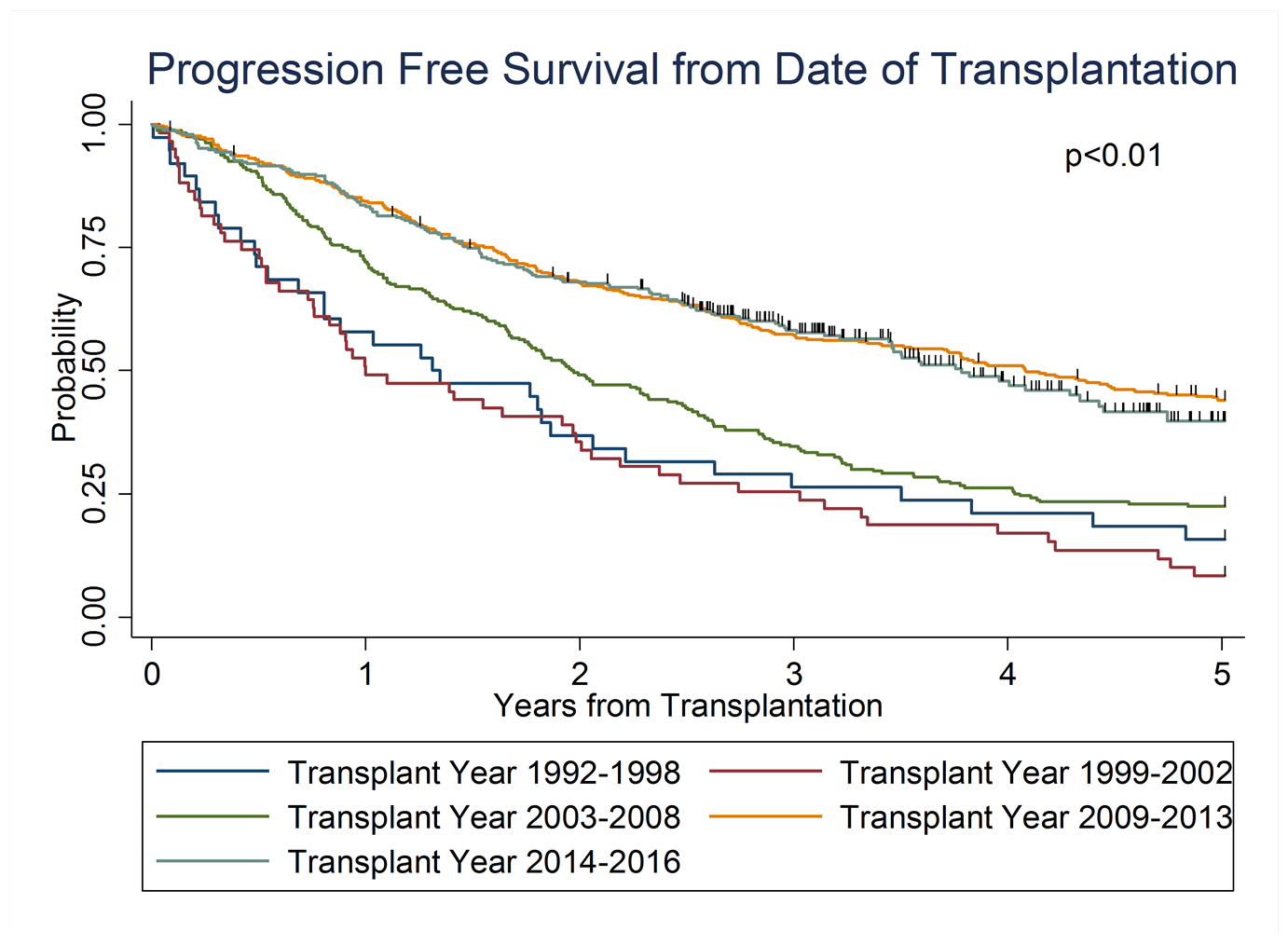
As Jordan explains, “Our data show that NDMM patients' survival and response to standard of care treatment have improved dramatically since 1992, primarily due to inclusion of novel therapies and maintenance [drugs]. For NDMM patients receiving ASCT, the 3-year overall survival rate has significantly improved from 45% in 1992-1998 to 80% in 2014-2016. The significantly increasing age of NDMM patients receiving ASCT over time suggests improving supportive care and expansion of standard of care therapies to more of the population, improving survival and quality of life.”
In measures of progression free survival (PFS), length of time to progressive disease or relapse increased, as did overall survival (OS), or time from transplantation to death from any cause, indicating an improvement in MM outcomes over time.
Jordan says he feels fortunate to match his interest in cancer research with the work that his physician preceptor and research mentor Dr. Yvonne Efebera and her team are doing. An Associate professor of hematology and Blood and Marrow Transplant at The Ohio State University Comprehensive Cancer Center, and a specialist in multiple myeloma research and treatment, Dr. Efebera was a key member of Jordan’s research team, providing guidance and support along the way.
While not curable, advances in the treatment of Multiple Myeloma, ASCT and maintenance therapy, such as those tracked in this study, have dramatically improved PFS and OS rates in recent years. The Ohio State University bone marrow transplant program has been using ASCT for NDMM patients since 1992. Jordan is hopeful that this work will not only broaden the understanding of bone marrow cancers like multiple myeloma, but provide a foundational database upon which to build future studies in the field.