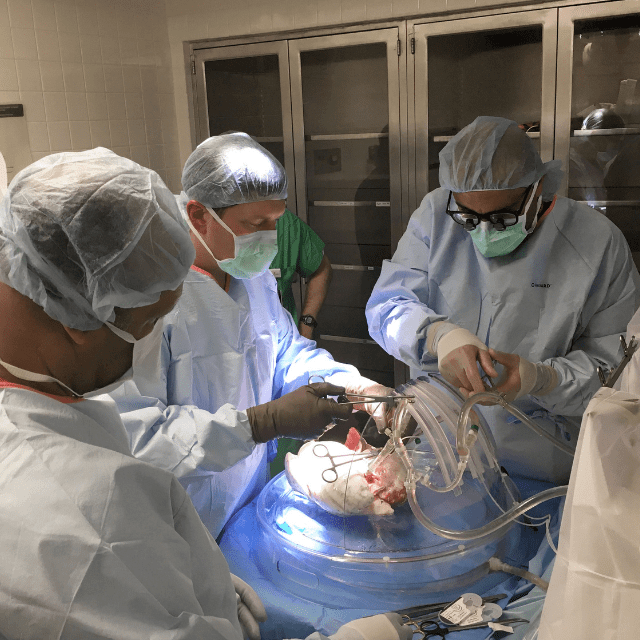
 A successful transplantation doesn’t happen in isolation.
A successful transplantation doesn’t happen in isolation.
“Completing the volume of transplants that we do shows the quality of our upstream and downstream care,” Bryan Whitson, MD, PhD says.
“Upstream, there’s effective organ procurement and a robust team caring for patients with critical conditions or end-stage diseases, keeping them healthy long enough to even make it to transplant.”
Among the advanced treatments Ohio State offers is extracorporeal membrane oxygenation, or ECMO, also known as extracorporeal life support. This artificial heart and lung machine oxygenates a patient’s blood outside the body and provides short-term support for patients with a failing heart and/or lungs.
“Downstream, there are our critical care units and the specialists who help transition patients to the lifelong care needed after discharge,” Dr. Whitson says. “It’s this multidisciplinary coordination of care that has established us as a regional referral center.”
One advancement that he highlights is ex vivo lung perfusion (EVLP), which Ohio State first used in 2016 as a participant in the landmark NOVEL Extension trial. EVLP is now routinely used to resuscitate and reevaluate donor lungs of questionable quality prior to transplantation. This single innovation means that donor lungs that wouldn’t have been accepted even 10 years ago are now being used at Ohio State to save more patient lives.
In addition, even in cases where EVLP isn’t used, the Ohio State Comprehensive Transplant Center’s organ procurement specialists are able to assess donor lungs in situ, confirming lung quality and function prior to accepting them. The result has been a median wait time for lung transplantation at Ohio State of just under one month.
Dr. Whitson notes that even after stretching the historic boundaries of donor lung recruitment using EVLP and more advanced organ procurement, Ohio State’s team consistently achieves strong patient outcomes. Data released by the Scientific Registry of Transplant Recipients in January 2023 confirms this for both the lung and heart transplant programs.
The complex critical care provided after surgery is crucial for this statistic, as is the program’s ability to reduce the risk of rejection using induction immunotherapy, rigorous antibiotic prophylaxis, scheduled surveillance bronchoscopies with biopsies to screen for rejection and ongoing monitoring for other types of rejection responses, such as antibody-mediated rejection.
Today, the Ohio State Comprehensive Transplant Center ranks in the top 20 nationally for lung transplantation volume.
“We do have tremendous capacity,” Dr. Whitson says. “But our team takes on each patient knowing we have a tremendous duty to care for them the rest of their life. It’s not a responsibility we take lightly. We’re here to provide the personalized care they deserve with any specialist they might need going forward.”
