Department of Surgery and School of Health and Rehabilitation Sciences collaborate to study effects of abdominal core rehabilitation after ventral hernia repair
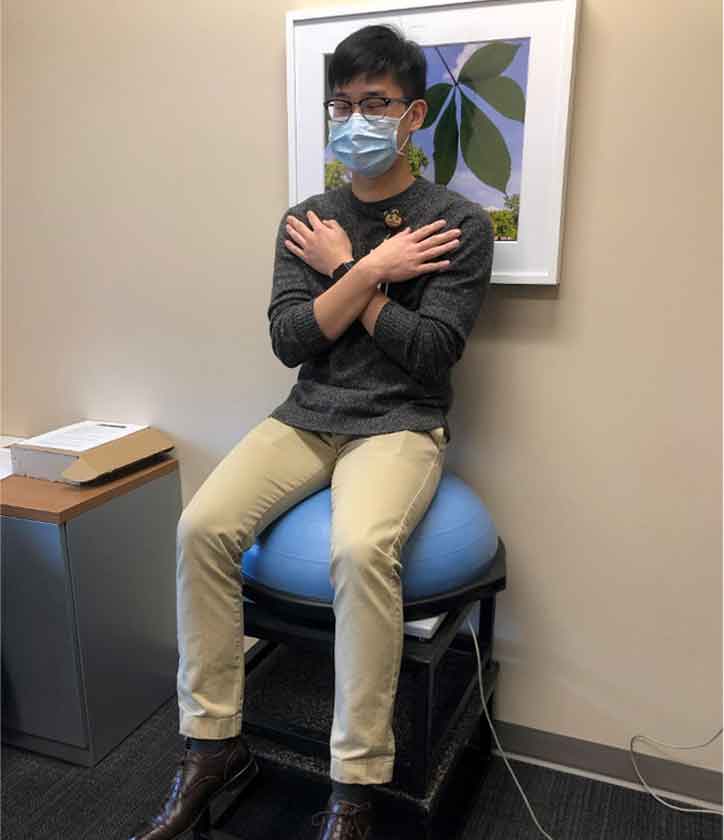
Hernia disease is one of the most common disruptions to the abdominal core and is caused when an opening in the abdominal wall causes pain or functional limitation. There has been a steady increase in the need for surgical repairs of hernias, with around 350,000 surgeries being performed in the United States each year. Unfortunately, the failure rate of these repairs ranges from 24%-43% due to reinjury, other diseases or a poorly maintained abdominal core.
In an effort to understand and mitigate this high failure rate, The Ohio State University College of Medicine’s Department of Surgery and the Ohio State School of Health and Rehabilitation Sciences have partnered to study the effects of abdominal core rehabilitation through physical therapy on the outcomes of ventral hernia repair. Through this research, they will begin a pilot trial focused on how to best rehabilitate the core musculature post surgery.
This research sees Benjamin Poulose, MD, MPH, professor of Surgery, partnering with Stephanie Di Stasi, PhD, PT, assistant professor of Health and Rehabilitation Sciences, and Ajit Chaudhari, PhD, professor of Health and Rehabilitation Sciences, to test the outcomes of patients who undergo the Abdominal Core Surgery Rehabilitation Protocol developed by the Abdominal Core Health Quality Collaborative. It took the work of five institutions over the past four years to establish the protocol, which asserts that maintenance of the abdominal core as a functional group is required for better surgical outcomes. The protocol calls for patients to undergo 10 weeks of rehabilitation after the hernia repair surgery, targeting abdominal core function through progressive muscle retraining and strengthening, and patient-specific posture and body mechanics education. Physical performance tests such as the established Five Times Sit-to-Stand, in which the time it takes a patient to stand is timed, and the Quiet Unstable Sitting Test, developed by this team of researchers, which tests the ability of a patient to self-stabilize, will act as measurements of patient recovery.
These measurements will be compared to patients in a control group, who will be given the current standard of care postoperative precautions.
“Physical therapy has historically been viewed as a complementary, but unnecessary, addition to routine orthopedic surgeries,” says Dr. Di Stasi. “In this trial, we think physical therapy, focused on the abdominal core, will emerge as a critical element of restorative care for patients with hernia care.”
Previous research has shown that functionality of the abdominal core does improve when subjected to strength and stability exercises.
“Previously, hernia repair was seen as a simple operation affecting only one area of the body,” says Dr. Poulose. “Over recent years, the concept of the abdominal core as a dynamic structure has gained acceptance.”
This clinical trial will be one of the first instances of formal research into hernia disease and abdominal core health funded by a National Institutes of Health (NIH) R01 grant.
“Due to the siloed nature of health care, there has been a lack of research in the fields of abdominal core health and hernia disease,” says Dr. Chaudhari. “The emphasis on interdisciplinary work in education and research at The Ohio State College of Medicine is what allows us to break out of these silos.”
The impacts of this study are significant considering that patients in the Abdominal Core Health Quality Collaborative’s national registry are frequently underperforming after surgery.
“Many patients are not as functional as those who haven’t had hernia disease,” says Dr. Chaudhari. “Because of this, there is room for improvement beyond merely avoiding repair failure.”
By exploring the impacts of physical therapy on patient outcomes, the study will provide valuable information on how to improve quality of life after ventral hernia repair.