Inherited variants in SCARB1 cause severe early-onset coronary artery disease
Coronary artery disease (CAD) is the most common form of heart disease in the United States. Often attributed to cholesterol-containing plaque buildup and inflammation, CAD killed more than 365,000 people in 2017. This buildup of plaque is known as atherosclerotic cardiovascular disease (ASCVD).
High-density lipoprotein-associated cholesterol (HDL-C) earns the “good cholesterol” nickname from its ability to sweep out other forms of cholesterol from the bloodstream, transporting it to the liver to be broken down and removed from the body. This process is referred to as reverse cholesterol transport. Several clinical trials have explored HDL-C elevation as a therapeutic, but the targeted mechanism was unsuccessful in improving ASCVD event risk.
Sara Koenig, PhD, assistant professor of Physiology and Cell Biology at The Ohio State University College of Medicine, hypothesizes that scientists should be targeting HDL metabolism, not HDL-C, based on the recent results of a study on HDL receptor SR-BI, a transmembrane receptor that facilitates cholesterol efflux and selective cholesterol uptake.
This hypothesis derived from her understanding that human variants in SCARB1, the protein coding gene for SR-BI receptors, were associated with abnormally elevated cholesterol levels. Dr. Koenig wanted to determine if heterozygous variants in this gene could be a cause of CAD.
Dr. Koenig studied the nucleic acid sequence of two brothers presenting severe premature CAD. She also studied their mother, who partially expressed the severe, early-onset CAD phenotype. She found that both brothers harbored compound heterozygous variants of SCARB1, inheriting one allele from their mother and one from their father.
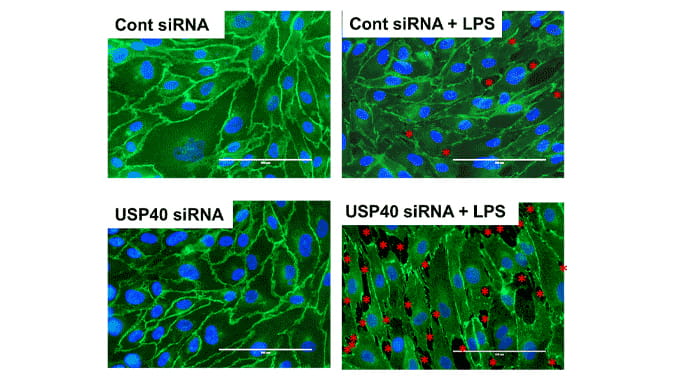
To get a better understanding of how the variant allele contributed to ASCVD and CAD, Dr. Koenig sourced induced pluripotent stem cells (IPSCs) from the two brothers, differentiating the IPSCs into hepatocyte-like cells, or liver cells. This procedure was done to study the expression of SCARB1 and cholesterol processing.
Her observations suggested that the variant maternal allele was not expressed in the patients, likely indicating a total reduction of the body’s access to HDL receptors, or SR-BI bioavailability. The variant on the paternal allele presented decreased cholesterol uptake, decreased HDL binding on the SR-BI receptor and greater affinity for dimerization. These observations suggest that this specific variant could be pathogenic in heterozygous individuals, or individuals with a normal second allele in their allele pair.
After using these observation to categorizing this variant SCARB1 as pathogenic, Dr. Koenig found the altered function of the resulting SR-BI receptor to have pernicious effects.
To further explore the full effects of this variant, Dr. Koenig created a mouse model that contained the variant gene sequence, and observed the effects of a defective SR-BI receptor. She found that homozygous knock-in mice suffered lethality by greater than 95%. This supported the pathogenicity of this variant.
“Our findings substantiate a causative role for SR-BI in severe inherited atherosclerotic disease,” says Dr. Koenig. “The defective SR-BI receptor results in the ineffective binding and uptake of HDL-C. These findings are supported by the homozygous lethality and heterozygous dyslipidemia, or abnormal cholesterol elevation, in a knock-in mouse model harboring the same mutation as the patients.”
Dr. Koenig’s work supports further investigation into HDL-mediated therapies of ASCVD.
“HDL has three key functions to consider for targeted therapies,” says Dr. Koenig. “Cholesteryl ester transfer to intermediate density lipoprotein via cholesteryl ester transfer protein, cholesterol efflux and cholesterol uptake.”
Dr. Koenig explains that future research should focus on reverse cholesterol transport.
“Clinical trials did not have success with improving outcomes of cardiovascular events with cholesteryl ester transfer protein inhibition, likely because this mechanism does not have an effect on cholesterol efflux or excretion,” says Dr. Koenig. “Future studies should consider investigating the therapeutic potential of augmenting reverse cholesterol transport to improve these functions.”
Dr. Koenig’s work reveals the first causative relationship between SCARB1 variants and the presentation of severe, early-onset CAD. Further, her findings open doors in the exploration of HDL metabolism as a therapeutic target for dyslipidemia and ASCVD.