Ohio State researcher turn easy-to-obtain urine cells to stem cells
A team of researchers at The Ohio State University College of Medicine has found a way to create stem cells out of cells that are obtained easily from a donor’s urine sample. The technique holds promise for fellow researchers who are looking for more efficient, safe and reliable methods to create stem cells that can be used to test therapies, as well as for physicians who want to better understand their patients’ disorders and how to treat them.
Led by Hua Zhu, PhD, associate professor of Surgery in the Division of Cardiac Surgery at Ohio State College of Medicine, the team collects and manipulates somatic or “adult” cells from urine and reprograms them into induced pluripotent stem cells (iPSCs) — cells that, like embryonic stem (ES) cells, have the ability to differentiate into many different types of cells, a necessary ingredient for use in regenerative cell therapy and drug screening. Dr. Zhu and his team generate cardiomyocytes or human heart muscle cells from urine-derived cells and manipulate them in the lab to advance their understanding of the cells’ properties and functions and to aid in the development of novel cell therapies.
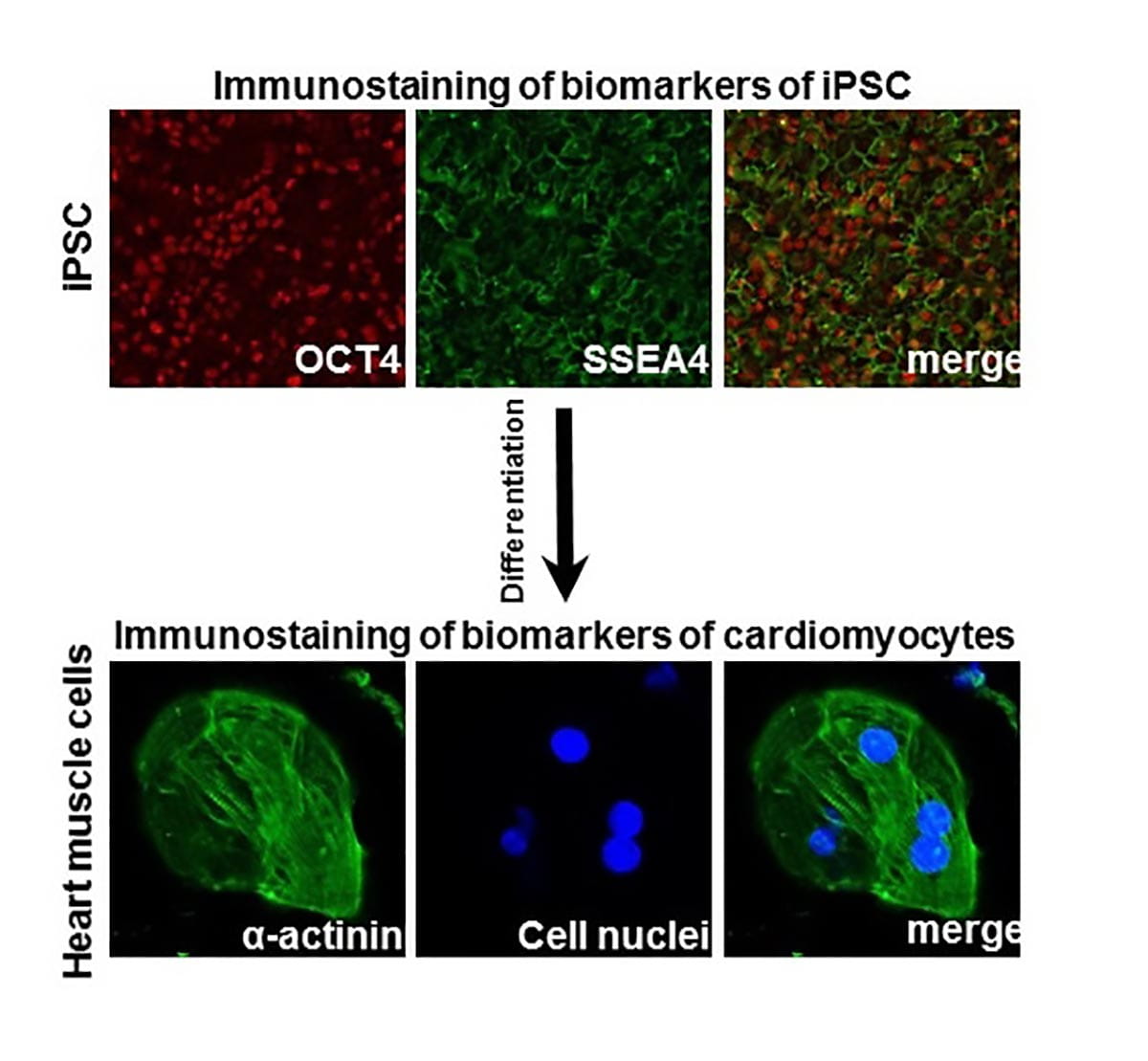 The team has established protocols introducing Yamanaka Factors Oct3/4, Sox2, Klf4, c-Myc, which are highly expressed in ES cells, into the somatic cells (see figure, upper panels) and further differentiating them into beating human heart muscle cells (see figure, lower panels). The team then uses a multiple-electrode array device to capture and record the electrical impulses that contract within each of the living cardiomyocyte cells — much the way an EKG functions — and identifies the cell’s contracting and electrophysiology properties, “essentially creating a beating heart in a dish,” explains Dr. Zhu.
The team has established protocols introducing Yamanaka Factors Oct3/4, Sox2, Klf4, c-Myc, which are highly expressed in ES cells, into the somatic cells (see figure, upper panels) and further differentiating them into beating human heart muscle cells (see figure, lower panels). The team then uses a multiple-electrode array device to capture and record the electrical impulses that contract within each of the living cardiomyocyte cells — much the way an EKG functions — and identifies the cell’s contracting and electrophysiology properties, “essentially creating a beating heart in a dish,” explains Dr. Zhu.
“The ability to reprogram somatic cells in the lab into pluripotent iPSCs that are functionally similar to ES cells and that can differentiate into the type of cells we want to study presents an exciting opportunity for further research and, ultimately, for the development of novel and personalized patient therapies,” he says.
In fact, Dr. Zhu and his team have already expanded their use of the technique in collaborations with other scientists and physicians at the medical center to study and reprogram the cells of patients whose cells carry various unique genetic mutations that cause diseases, such as muscular dystrophy and cancer, creating a pathway for the development of new therapies for these patients.
“Working at Wexner Medical Center has so many advantages for researchers like me who are interested in stem cell research and its therapeutic potential because of the breadth and variety of disease types that are available for study,” says Dr. Zhu. “Doctors here are realizing the therapeutic advantages of being able to collaborate with researchers in the lab who have the ability to generate iPSCs that are identical to the cells in the bodies of some of their patients.”
The use of this new technology in preclinical testing and in vitro models promises to improve success rates in the drug development process by providing data that is much more reliable and efficient than data obtained from other methods.
“Since we are working in the lab with a model that provides accurate data allowing for exact replication of a particular donor’s cell structure and function, we are able to test therapies as personalized treatment options to fit the way that particular person’s disease is expressed,” he concludes.