Ohio State receives $4.1 million grant to lead multicenter cochlear implant study
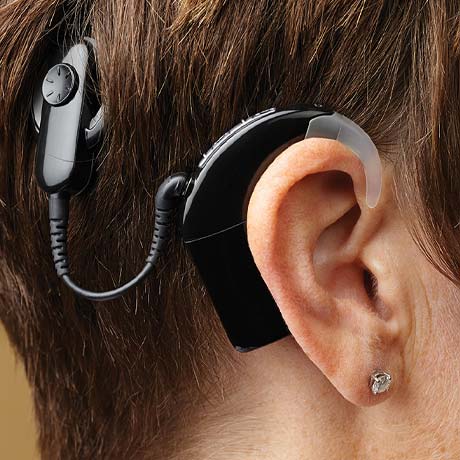 Researchers at The Ohio State University College of Medicine will lead a five-year, $4.1 million multicenter project to study the clinical utility of residual hearing in the cochlear implant (CI) ear.
Researchers at The Ohio State University College of Medicine will lead a five-year, $4.1 million multicenter project to study the clinical utility of residual hearing in the cochlear implant (CI) ear.
The grant, a prestigious National Institutes of Health U01 research project cooperative agreement, was awarded to seven U.S. centers—Mayo Clinic, Medical College of Wisconsin, The Ohio State University College of Medicine, University of North Carolina, Vanderbilt University and Washington University.
Oliver Adunka, MD, the William H. Saunders, MD, Professor of Otolaryngology at Ohio State College of Medicine and principal investigator of this study, is thrilled about this collaboration. “The centers were chosen based on their cochlear implant volumes and their expertise in hearing preservation. They are truly leaders in the field,” he says.
These leaders will work together to study a major concern in CI: the loss of residual hearing associated with surgery. Many candidates are faced with the decision to relinquish their remaining acoustic hearing in exchange for electric hearing via the CI. A potential solution is a stimulation strategy called electric acoustic stimulation, which has been used to describe the ipsilateral combination of electric hearing via a CI and acoustic hearing via a hearing aid. This requires preservation of residual hearing, which is currently possible but inconsistent.
Dr. Adunka has been working on hearing preservation cochlear implantation since the late 1990s. Over the past 15 years, he has developed a new technology to potentially improve hearing preservation—intraoperative electrocochleography (ECochG)—which has recently been implemented into commercially available CI systems. Dr. Adunka hopes ECochG will improve hearing preservation and thus overall outcomes with CIs.
The team will test the new technology by enrolling and randomizing patients with substantial levels of hearing loss who qualify for electric acoustic stimulation. Subjects will receive either intraoperative ECochG monitoring or conventional CI electrode insertions. Hearing preservation and other performance outcomes will be recorded and analyzed between the groups to assess the clinical value of intraoperative monitoring and hearing remnants in combination with the implant.
The study aims to discover whether CI electrode insertion based on ECochG is better for achieving hearing preservation and whether electric acoustic stimulation is better than conventional CI among electric acoustic stimulation candidates. Ultimately, the outcomes of this clinical trial will provide an evidence-based clinical guide for electrode insertions, broaden candidate pool by including patients with greater levels of residual hearing, and potentially improve outcomes following CI.
Dr. Adunka is eager to get started. “This clinical trial is really the culmination of two decades of work where we will answer questions central to driving the clinical care of future cochlear implant recipients.”



