What is an SP?
Traditionally, ‘SP’ refers to Standardized Patients or Simulated Patients. But SPs are not limited to medical simulations. SP may refer to Simulated Participants, Simulated Professionals, Simulated Parents, and many other permutations.
SPs are specifically recruited and trained with realistic case materials to often portray a patient in simulated encounters accurately and consistently. Our program provides the opportunity for learners to exercise their patient care and communication skills through role playing and receiving feedback. These experiences are designed to fill the gap between learning in the classroom and real-life interactions. We believe students learn best through practice and experience.
Simulated interactions between a learner and SPs offer a standardized, controlled experience for learners. Interactions are measurable and reproducible, unlike peer role-play or the use of actors or volunteers who have not received our program’s high-quality and nationally recognized SP training.
SP methodology is based on Association of SP Educators (ASPE)’s Standards of Best Practice. SP methodology is additionally recognized by the Liaison Committee on Medical Education (LCME) and the Accreditation Council for Graduate Medical Education (ACGME) as a valid, reliable tool for training and evaluation in the undergraduate and graduate medical education settings.
Are SPs limited to only medical simulations?
No! In fact, our SP program is very robust and easily adaptable to your program’s needs.
‘SP’ may stand for other roles such as ‘Simulated Person’, ‘Simulated Parent’, ‘Simulated Participant’, and other similar terms. The term SP is not meant to be limiting, but it is an industry-standard title.
Our SPs can adapt and be trained for any standardized or simulated interaction you may need. Examples of SP portrayals may include a grieving family member, a cat’s owner, a graduate student receiving performance feedback, a law firm’s client, and so many other such roles. Our SP team will work with your program to best meet your needs.
The use of SPs facilitates practice in critical thinking, patient safety, crisis management, team interaction, decision making and communication skills in addition to acquisition of competence in clinical techniques and procedures.
Who are the SPs?
The pool of highly trained SPs come from many backgrounds and walks of life, such as education, medicine, finance, law enforcement, acting, and social work. SPs represent a wide range of demographics in age, ethnicity, gender, sexuality, physical ability, and more.
We pride ourselves on the values found in the SPs. These include:
- Punctual
- Flexible and adaptable
- Maintain confidentiality
- Trained in quality evaluation and feedback
- Consistent and reliable role portrayal
Frequently Asked Questions
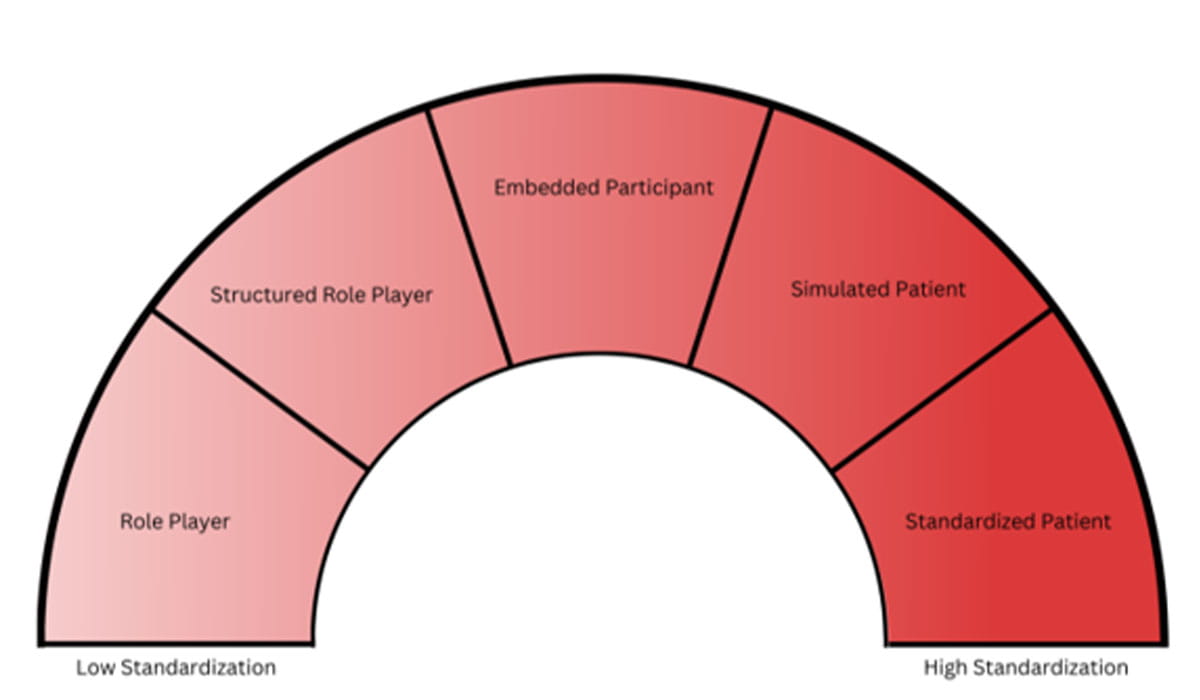
- Standardized Patient (or Participant/Person): Individuals who are trained to portray a patient with a specific condition in a realistic, standardized and repeatable way (where portrayal/presentation varies based only on learner performance and are trained to behave in a highly repeatable or standardized manner to give each learner a fair and equal opportunity).
- Simulated Patient (or Participant/ Person): A person who has been carefully coached to simulate an actual patient so accurately that the simulation cannot be detected by a skilled clinician. In performing the simulation, the SP presents the “Gestalt” of the patient or participant being simulated; not just the history, but the body language, the physical findings and the emotional and personality characteristics as well. These roles may vary somewhat between encounters, with a bit of improv used based off the learner’s actions.
- Embedded Participant/Person: An individual who is trained or scripted to play a role in a simulation encounter in order to guide the scenario based on objectives. This may include portraying a nurse, a security guard, or other similar roles.
- Structured Role Play: A person who has been provided a prepared script on one element of a scenario which articulates a learning objective. Improvisation meets structure.
Role Player: Asking someone to imagine that they are either themselves or another person in a particular situation. Role Players behave exactly as they feel that person would, and thus do not need a case developed.
- Located in Prior Hall
- Started in 2004
- We support the Colleges of Medicine, Nursing, Dentistry, Occupational and Physical Therapy, Health and Rehabilitation, Pharmacy, Veterinary Medicine, Social Work, and Communications.
- We support programs such as Genetic Counseling, Nutrition and Dietetics, and the office of Interprofessional Practice.
- We also work with the OSU Wexner Medical Center’s Residency programs, such as Emergency Medicine, Anesthesia, Family Medicine, Internal Medicine, and Neurology.
- Additionally, we work with several external organizations such as Nationwide Children’s Hospital and the Ohio Department of Health.
- Programming is tailored to align with specific disciplinary and curricular objectives, while maintaining industry best practices and ensuring high precision in every event.
The SP program is accredited by the Association of SP Educators (ASPE)*
- Standardized Patients with the College of Medicine, including in high-stakes objective structured clinical examinations (OSCEs)
- Physical Exam Teaching Associates (PETAs) with the College of Medicine, which includes a teaching component in addition to assessing physical exam skills
- Stroke patients
- Simulated Nurses
- Simulated family members in medical emergencies
- Simulated residents, fellows, respiratory therapists, medical assistants, doctors, and other medical professionals
- Simulated clients for veterinary medicine (pet ‘parents’ or owners)
- Physical exam models for non-invasive exams
- Physical exam models for invasive sensitive (breast/pelvic) exams
- Physical exam models for ultrasound
- And so many more!
SPs are paid an hourly wage and there is no required qualifications, acting or medical experience to apply. The Clinical Skills Education and Assessment Center hires and trains a comprehensive group of SPs. We strongly encourage anyone age 18+ of any racial, ethnic, or religious background, as well as those of any ability, gender, or sexual orientation to apply.
Being an SP requires active listening skills and concentration while being interviewed and examined. You must be able to maintain accuracy regarding the patient's history as well as simulate physical condition during an encounter. When the encounter is over, you must recall the student's performance and record it on an evaluation form. You will repeat these tasks many times in succession without change. Being an SP takes energy, memorization, discipline, concentration, and excellent communication skills. It is important that you are comfortable with your body and letting others touch and examine you. Strong written and verbal communication skills are required. Ideal candidates have a desire to participate in healthcare education, have the ability to learn how to consistently simulate patient cases, and posses personal dependability.
After reviewing your application one of our program coordinators will reach out to schedule you for our next upcoming orientation. Orientation for new SPs is scheduled according to availability. Once a new SP is added to the program most of the events occur during the academic year (August-May). Typically, events are scheduled during business hours, Monday through Friday.
The SP Program is located in the Clinical Skills Education and Assessment Center, located in the lower level of Prior Hall.
