Greetings from the Director
As we approach the holiday season and the cold and snowy weather, we at DMRC would like to send you our warmest wishes. Many of us celebrate the holiday season by hanging a kwanza wreath, going to midnight mass, lighting the menorah, making New Year’s resolutions, looking forward to Chinese New Year or just enjoying some time off work. However, for all of us, it’s an opportunity to stop and reflect on the people who give our lives meaning. I want to take the opportunity to say a hearty "Thank you" to our patients, our community, our partners, our colleagues, and our friends for your continuous support and dedication. You are the reason we strive toward our vision of "to prevent and cure diabetes, obesity, and metabolic disease through innovative research and discovery."
I am thrilled to share that our annual Diabetes Research and Education Update "Dining for Diabetes" event was a success and was attended by over 200 guests, including the Dean Carol Bradford of the Wexner College of Medicine; Dr. Rama Mallampalli, Chair of the Department of Internal Medicine; Dr. Timothy Pawlik, Chair of the Department of Surgery. Our special guest was Nicole Johnson, Miss America (1999) who vividly described how she conquered type 1 diabetes to win “the crown.” Our DMRC honoree was Mr. Dax Dyson, who cured himself of type 2 diabetes and has not required medication for nearly two years. The event was hosted by fabulous Angela An, a 6-time Emmy Award-winning journalist and anchor of WBNS-10TV. The primary goals of the Diabetes Education and Research Update dinner event were to focus on highlights from the past year of innovative research, share the future goals of the Diabetes and Metabolism Research Center (DMRC), and in addition, to bring together community partners and medical professionals as well as friends to develop possible strategies to make the world free of diabetes. The event was truly inspirational!
I am excited to share that our next DMRC event will be the Annual Islet Cell Invitational at Columbus Country Club. More details to come. We hope that we are able to host this event during warmer weather. Please see below some of pictures from past Golf event.
Have a happy and safe holiday season!
Best wishes,
Willa Hsueh, MD
Director, Diabetes and Metabolism Research Center
Division of Endocrinology, Diabetes and Metabolism

Researcher Spotlight
 Martha Ann Belury, PhD, RDN
Martha Ann Belury, PhD, RDN
Dr. Martha Belury is the Carol S. Kennedy professor of human nutrition in the Department of Human Sciences. Her research interests are investigating the mechanisms of bioactive lipids in regulating insulin sensitivity in liver, adipose and muscle, and the role of energy balance in cancer prevention.
In the News
“Ohio man appears to be first in the world to be cured of Type 1 diabetes”
A northeast Ohio man has a whole new grasp on life while making medical history after the successes of participating in a clinical trial. Type 1 diabetes has controlled Brian Shelton’s life for more than 40 years. He was diagnosed at the age of 21. As he aged, the autoimmune disease became harder to control. He’s what doctors called a brittle diabetic, meaning his blood sugar swings were severe and frequent.
Research Updates
“Insulin expression and C-peptide in type 1 diabetes subjects implanted with stem cell-derived pancreatic endoderm cells in an encapsulation device”
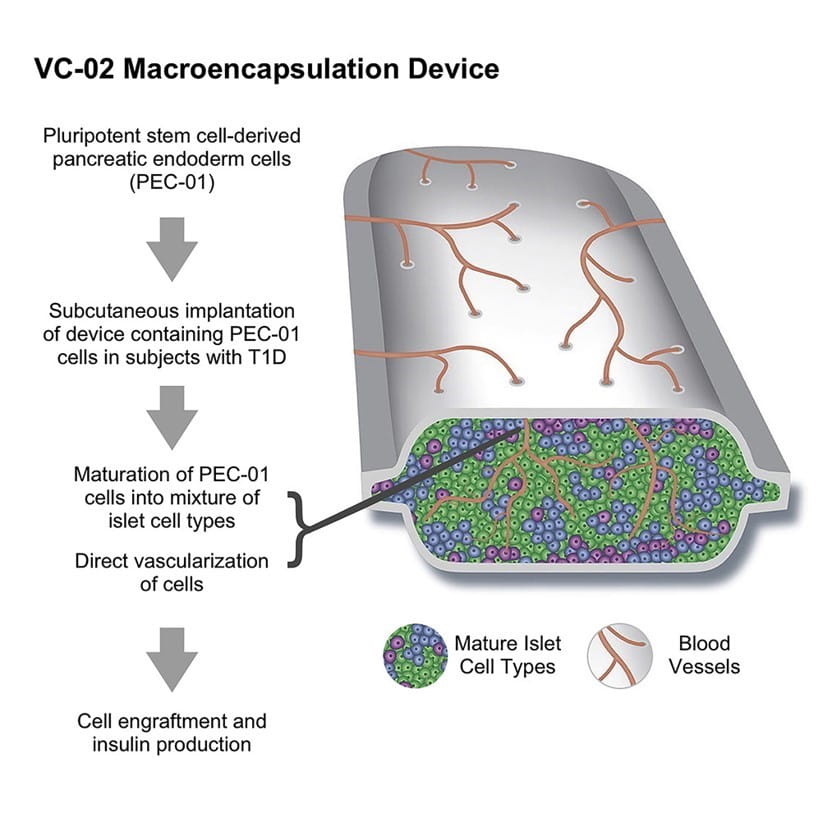 Approximately 100 years since the discovery of insulin, type 1 diabetes (T1D) remains a life-altering and sometimes life-threatening diagnosis. While insulin is lifesaving, it fails to prevent progression of end-stage microvascular complications in many subjects, and imprecision with insulin delivery often results in hypoglycemia and glycemic lability. Modern insulin delivery systems include advances in insulin pumps, continuous glucose monitoring, and glucose-responsive systems, but these advances fail to prevent hypoglycemia, do not consistently enable subjects to achieve glycemic targets, are burdensome to wear for protracted periods, and can malfunction. Further, even with careful administration of exogenous insulin, long-term complications are common. Cell-based therapy may ultimately offer a more effective alternative to injected insulin. Over the past 20 years, islet transplantation has provided important proof-of-concept that restoring internally regulated insulin and glucagon production is a safe and effective treatment option for selected subjects with difficult- to-control T1D. Islet cell transplantation with concomitant immunosuppression can lead to clinically relevant endogenous insulin secretion.1,2,3 A few islet allograft recipients have maintained insulin-independence for over 20 years duration, but most return over time to needing minimal-to-moderate exogenous insulin administration.
Approximately 100 years since the discovery of insulin, type 1 diabetes (T1D) remains a life-altering and sometimes life-threatening diagnosis. While insulin is lifesaving, it fails to prevent progression of end-stage microvascular complications in many subjects, and imprecision with insulin delivery often results in hypoglycemia and glycemic lability. Modern insulin delivery systems include advances in insulin pumps, continuous glucose monitoring, and glucose-responsive systems, but these advances fail to prevent hypoglycemia, do not consistently enable subjects to achieve glycemic targets, are burdensome to wear for protracted periods, and can malfunction. Further, even with careful administration of exogenous insulin, long-term complications are common. Cell-based therapy may ultimately offer a more effective alternative to injected insulin. Over the past 20 years, islet transplantation has provided important proof-of-concept that restoring internally regulated insulin and glucagon production is a safe and effective treatment option for selected subjects with difficult- to-control T1D. Islet cell transplantation with concomitant immunosuppression can lead to clinically relevant endogenous insulin secretion.1,2,3 A few islet allograft recipients have maintained insulin-independence for over 20 years duration, but most return over time to needing minimal-to-moderate exogenous insulin administration.
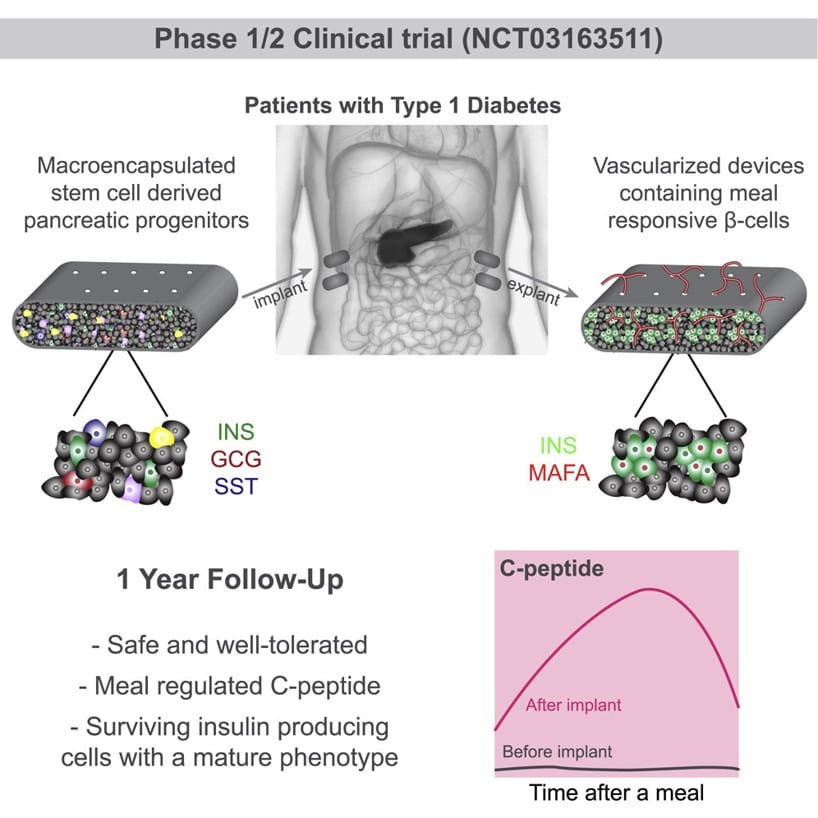 The most durable benefit of islet transplantation has been elimination of severe hypoglycemia while normalizing hemoglobin A1c (HbA1c) in high-risk subjects.2,3 The preliminary data from an ongoing first-in-human phase 1/2, open-label study provide proof-of-concept that pluripotent stem cell-derived pancreatic endoderm cells (PEC-01) engrafted in type 1 diabetes patients become islet cells releasing insulin in a physiologically regulated fashion. In this study of 17 subjects aged 22- 57 with type 1 diabetes, PEC-01 cells were implanted subcutaneously in VC-02macroencapsulation devices, allowing for direct vascularization of the cells. Engraftment and insulin expression were observed in 63% of VC-02 units explanted from subjects at 3–12 months post-implant. Six of 17 subjects (35.3%) demonstrated positive C-peptide as early as 6 months post-implant. Most reported adverse events were related to surgical implant or explant procedures (27.9%) or to side-effects of immunosuppression (33.7%). Initial data suggest that pluripotent stem cells, which can be propagated to the desired biomass and differentiated into pancreatic islet-like tissue, may offer a scalable, renewable alternative to pancreatic islet transplants. Ohio State Wexner Medical Center was and continues to be a part of this state-of-the-art trial. For inquiries, please contact Dr. Kathleen Dungan and the OSU research coordinators at 614-688-6257.
The most durable benefit of islet transplantation has been elimination of severe hypoglycemia while normalizing hemoglobin A1c (HbA1c) in high-risk subjects.2,3 The preliminary data from an ongoing first-in-human phase 1/2, open-label study provide proof-of-concept that pluripotent stem cell-derived pancreatic endoderm cells (PEC-01) engrafted in type 1 diabetes patients become islet cells releasing insulin in a physiologically regulated fashion. In this study of 17 subjects aged 22- 57 with type 1 diabetes, PEC-01 cells were implanted subcutaneously in VC-02macroencapsulation devices, allowing for direct vascularization of the cells. Engraftment and insulin expression were observed in 63% of VC-02 units explanted from subjects at 3–12 months post-implant. Six of 17 subjects (35.3%) demonstrated positive C-peptide as early as 6 months post-implant. Most reported adverse events were related to surgical implant or explant procedures (27.9%) or to side-effects of immunosuppression (33.7%). Initial data suggest that pluripotent stem cells, which can be propagated to the desired biomass and differentiated into pancreatic islet-like tissue, may offer a scalable, renewable alternative to pancreatic islet transplants. Ohio State Wexner Medical Center was and continues to be a part of this state-of-the-art trial. For inquiries, please contact Dr. Kathleen Dungan and the OSU research coordinators at 614-688-6257.
Please visit: Cell Reports Medicine, December, 2021, to read the full article “Insulin expression and C-peptide in type 1 diabetes subjects implanted with stem cell-derived pancreatic endoderm cells in an encapsulation device”.
From the Clinic
Traveling With Diabetes
Diabetes can make everyday life and travel more challenging, but it doesn’t have to keep you close to home. The more you plan ahead, the more you’ll be able to relax and enjoy all the exciting experiences of your trip. Traveling to new places gets you out of your routine and that’s a big part of the fun. But delayed meals, having unfamiliar food, being more active than usual, and being in different time zones can all disrupt your diabetes management. Plan ahead so you can count on more fun and less worry on the way and when you get to your destination. Before traveling, visit your doctor for a checkup to ensure you’re fit for the trip.
Ensure with your doctor that your trip is safe and ask these questions:
- How your planned activities could affect your diabetes and what to do about it.
- How to adjust your insulin doses if you’re traveling to places in a different time zone.
- To provide prescriptions for your medicines in case you lose or run out of them.
- If you’ll need any vaccines.
While you are traveling make sure to stop and get out of the car or walk up and down the aisle of the plane or train every hour or two to prevent blood clots (people with diabetes are at higher risk). Set an alarm on your phone for taking medicine if you’re traveling across time zones. Check your blood sugar often and treat highs or lows as instructed by your doctor or diabetes educator. See graphic
For more tips for travel with diabetes please visit:
https://www.cdc.gov/diabetes/library/features/traveling-with-diabetes.html
https://www.tsa.gov/coronavirus
Diabetes and Depression
The rate of depression in people with diabetes is much higher than in the general population. Women experience depression about twice as often as men, and the risk of depression increases in women with diabetes. People with type 1 and type 2 diabetes are at a heightened risk of mental health issues such as diabetes distress, depression, anxiety, and disordered eating. In particular, depression is more prevalent during the winter months. Additionally, lack of enough sunlight can trigger the symptoms of depression to be more vivid. However, these are all treatable disorders. It is important to pay attention to your feelings about having diabetes or taking care of someone who has diabetes. Talk to your physician, or your diabetes educator, or anyone you feel comfortable with on your diabetes care team. They can help you connect to mental health care, whether it is with a counselor, a therapist, a psychiatrist, or a social worker. Having support while living with diabetes is essential. Sometimes, talking to a friend with diabetes can also be helpful. We at DMRC here to help you if you need diabetes care or consultation.
Mental health care is an integral part of diabetes management, and the American Diabetes Association offers support and tools to help you tackle the day-to-day challenges (https://www.diabetes.org/healthy-living/mental-health). The ADA Mental Health Provider Referral Directory can help you locate mental health professionals in your area that have expertise in diabetes care. See graphic
Current Event
Vision for the Diabetes and Metabolism Research Center Type 1 DM and Beta Cell Biology Program
Healthy Cooking
 New recipes for healthier meals—in under 20 minutes!
New recipes for healthier meals—in under 20 minutes!
Join us live every month on the 2nd and 4th Tuesday at noon when Chef Katie McCurdy, BHS from the James Mobile Education Kitchen and Diabetes Care and Education Specialist Jenny C. Shrodes, RD, LD, CDCES bring you flavorful Diabetes Friendly Recipes, offer tips and tricks, and answer your questions about cooking with diabetes, all in under 20 minutes.
Low calorie, diabetes-friendly recipes, from our kitchen to yours:
Browse through our Garden to Table recipe book that emphasizes the fruits and vegetables that are key components of a healthy diet.

